(from Jenn)
I've seen such a variety of diagnoses during my short period of time here at Kibuye. I find myself reading more articles and textbooks now than I did even during residency. I love learning and I love this job. Some diseases are impossible to diagnose (ones where you need renal biopsies, or specific antibody or serologic testing for... which we don't have available here) while some, if you know what to order, are a joy to work through.
For example, we had child present with edema, hypertension, and cola-colored urine. We (the students and interns and I) worked through the differential diagnosis. On admission the doctor had asked for a study of the urine, but the lab stated the urine was to discolored and wouldn't work. So we worked through the differential - they considered nephrotic syndrome and congenital heart disease, renal insufficiency. I said that these were good ideas, but we should try again for a urine analysis. It came back the next day positive for blood (causing the cola-colored urine), but only mildly positive for protein. For the diagnosis of nephrOTIC syndrome, on expects to see A LOT of protein in the urine. So this diagnosis didn't quite fit. I asked the team to try to come up with another diagnosis to put on the differential. Someone suggested nephrITIC syndrome and I agreed. I asked the team if they knew one more test we could do to try to narrow down the diagnosis, and we decided to obtain an ASO titer. If positive, it tells you that the patient has had a recent infection with Group A Streptococcus (AKA the bug that causes strep throat and scarlet fever, which can eventually cause glomerulonephritis OR rheumatic heart disease). It came back positive. So we had the diagnosis - Post-streptococcal glomerulonephritis.
While most of the time it's fun to figure out a diagnoses, a class of diagnoses that are not so fun are congenital malformations concerning major organs that, here, result in rapid decline and death.
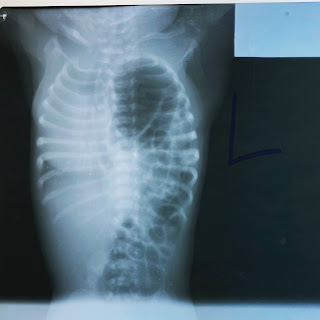
This baby was born at term or near term and had rather significant respiratory distress right after delivery and was therefore transferred to us in the NICU. The baby's distress did not improve, even with high amounts of oxygen so we decided to obtain an x-ray which showed this.
This is a large diaphragmatic hernia - where the diaphragm does not develop correctly leaving the possibility for the intestines and sometimes the spleen and kidney to enter into the chest area. This causes a problem because the lungs therefore cannot develop correctly. With many disease, there is a range of severity. Sadly for this baby, the lungs seemed to be quite underdeveloped which could not be fixed by a surgery.
Fortunately this is not the norm. More times than not, the NICU is full of babies born too early who need a little bit more time to grow and develop, who need to be closely monitored for infection and who need to live in a controlled setting before being able to go home.

1 comment:
This is really a tough case to handle the patient with some organ disorders and difficult to live. Ofcourse cancer is also dangerous even when the body structured well. Awareness of health has to be brought to every individual to make their life happy.
Post a Comment