by Jenn Harling
In February I wrote a blog describing what our neonatal unit looked like in our new pediatric building into which we moved at the end of 2021. I mentioned in that blog that I had attended a neonatal conference a few months prior (Oct 2022). I had the lovely opportunity to attend that conference again this year. This is not an ordinary neonatal conference, but rather one to bring together those who care for and treat neonates in Africa. I'll state the obvious in case it's needed - taking care of neonates in LMICs (Low and Middle Income Countries) in Africa is not the same as practicing neonatology in HICs (High Income Countries). This conference focuses on educating and training as well as sharing up-to-date information regarding neonatal care around the world, and also (and possibly more importantly) innovative ways to treat neonates when all the technology and resources are not available.
Not only is there a huge opportunity to learn, it's also a place to network and make connections as well aso talk to others who are also trying to find innovative solutions to challenges faced in a low-resource setting. I've met numerous people who are in similar settings and it is so helpful - "oh, do you have this challenge too? this is how we navigate this situation without _____ (insert resource that may not be available in LMICs like blood cultures, electrolytes, intubation, ventilators, IV pumps, arm boards, paging system, caffeine...).
I have left this conference each year thinking "there is SO much to do at our hospital to improve the care we provide..." but then I looked back and realized we have already started the process!
Below are a few things that changed in our unit after attending last year's conference:
-Trying to keep a cadre of nurses in the unit who do not rotate out.
-Hand hygeine
-Keeping a particular generalist doctor mostly in the unit when a specialist was not available to round.
-Updated feeding protocol with fortification of breastmilk
-Transfusion protocol to know when to transfuse neonates
-New neonatal ward manual in French being written
-more kangaroo mother care (skin to skin care), with hopes to increase even more this year
-humidification of oxygen
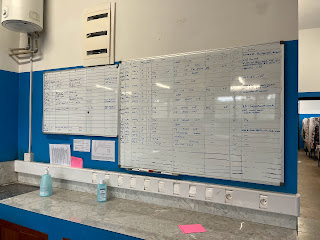
-patient tracking white board
-updated fluids management protocol
-hats for every baby in the unit