(From Alyssa): Through our two years in Kenya, we certainly were reminded daily of the gaps in our medical knowledge regarding tropical medicine and diseases, surgeries, etc. outside the scope of our American residency programs. We learned a lot from our Kenyan colleagues, from the long term missionaries, and from various continuing medical education activities. And thankfully God continued to show His strength in our weaknesses!
From a human perspective, so much additional training would be helpful for our work in Burundi - medical education, various subspecialties, community health, hospital administration, laboratory set up, ultrasound, seminary, etc., etc. For now we're all pursuing linguistic and cross cultural adaptation training (as mentioned in previous and future blogs at Mission Training International in Colorado), Sonship (Gospel transformation discipleship course), language learning (French and Kirundi), and Eric and I are participating in tropical medicine courses at two different sites this year. We look forward to seeing the partners God brings across our paths who have expertise in areas we lack and also to continuing to learn reliance on Him through our deficiencies.
All that to say, I'm currently in Peru for two months at the Gorgas Tropical Medicine course (see my blog on the right for more info & pictures about that) and I bring back to the McCropder blog the Case of the Week:
 |
| Half of my Gorgas classmates pictured with nurses from the clinic we visited this week |
So he has active pulmonary tuberculosis again. And this time, drug susceptibility testing was done. And as you see in the below medical chart, his tuberculosis is resistant to all but one of the first line TB drugs.
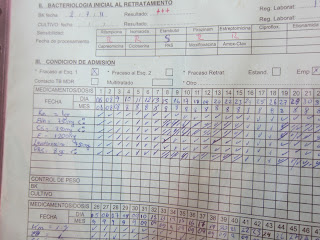 |
| Note the top of the picture: Smear positive tuberculosis resistant to almost all of the most used TB drugs - rifampin, isoniazid, pyrizinamide, and streptomycin |
This box contains the entire treatment course for our 19 year old patient. He comes daily for his medications including one injectable med and five oral meds. If he doesn't show up, someone from the clinic goes looking for him - and hopefully finds him unless he gave the wrong address (which is evidently common). This box of meds for one case of multidrug resistant TB costs about $5000. An entire 6 month course of first line meds for a susceptible TB patient costs about $20.
 |
| Our patient's daily six drug regimen |
 |
| Map of the world with proportion of tuberculosis cases per country |
It's estimated that worldwide only 7% of all multi-drug resistant TB cases are diagnosed (due to a lack of laboratory facilities, rapid tests, funding, etc.). But if you're a ministry of health official for a poor country and you can treat 250 susceptible tuberculosis patients for the price of 1 drug resistant patient, where do you put your efforts?



No comments:
Post a Comment